Figliozzi and Company
http://www.figliozzi.com/
There are 2 audit guides published by CMS, each very similar to one another and each offering some very basic information:
- Documentation must be retained for six years post-attestation
- CMS and its contractors will perform the audits on Medicate and dually-eligible providers
- States and their contractors will perform the audits on Medicaid providers
- Post-payment audits will be completed during the course of the EHR Incentive Programs
- Medicare audit notification will come from Figliozzi and Company, or the EHR Meaningful Use Audit Team
- CMS has an appeals process for eligible professionals that participate in the Medicare EHR Incentive Program
- The primary documentation that will be requested in all reviews is the source document(s) that the provider used when completing the attestation
- The initial review process will be conducted at the audit contractor’s location, using the information received as a result of the initial request letter
- States will have separate audit processes for their Medicaid EHR Incentive Program
- Once the audit is concluded, the provider will receive an Audit Determination Letter from the audit contractor
Not all certified EHR systems currently track compliance for non-percentage-based meaningful use
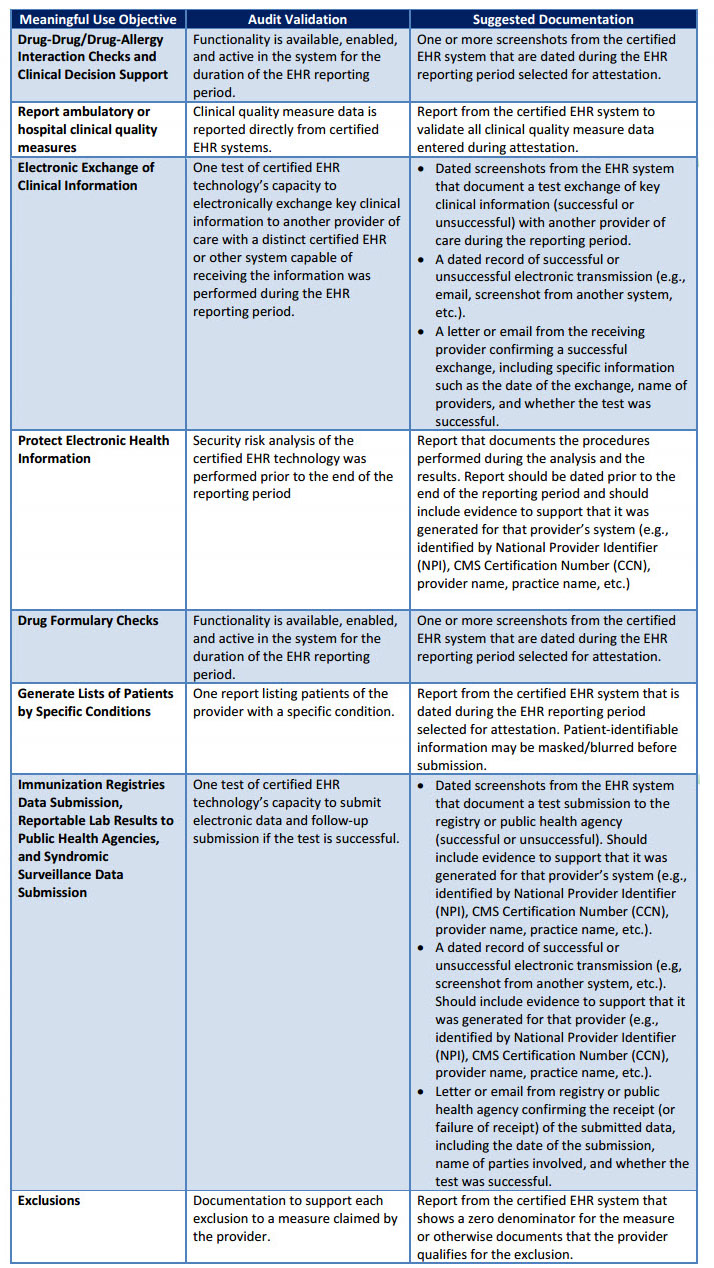
Objectives and these typically require a “Yes” attestation in order for a provider to be successful in meeting meaningful use criteria. Some software such as Greenway PrimeSuite go above and beyond with full dashboard devoted to helping practices know where they stand. In order to validate provider attestation for these objectives, CMS and its contractor may request further supporting documentation. Below is a chart from CMS explaining these items:
If an audit is failed there is an appeals process, but some are finding that the process is full of confusing roadblocks. Jim Tate, president of Asheville, North Carolina-based EMR Advocate and an expert in Meaningful Use audits and appeals recently wrote in a blog article, “Since I work with many EHs and EPs undergoing CMS EHR Incentive audits it is important that we know the rules. Back in 2011 and 2012 there was very little clarification from CMS on the issues of meaningful use and attestation. CMS admits there was much confusion and has adapted the program to alleviate some of these issues. Unfortunately the appeals process has not seen the benefit of corrective adjustment. In fact it seems to be getting worse.”
While an audit is bad enough, it appears that the appeals process is even worse as processes have not been completely figured out and formalized. Numerous examples have been cited by many professionals and all hope that the appeals process is spelled out soon.